OBESITY
Click the red to step ahead! Clink any of the red links below to read more about the topic.


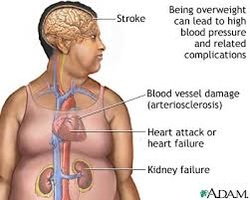


|

August 13, 2013 Obesity means having too much body fat. It is different from being overweight, which means weighing too much. The weight may come from muscle, bone, fat, and/or body water. Both terms mean that a person's weight is greater than what's considered healthy for his or her height. Obesity occurs over time when you eat more calories than you use. The balance between calories-in and calories-out differs for each person. Factors that might affect your weight include your genetic makeup, overeating, eating high-fat foods, and not being physically active. Being obese increases your risk of diabetes, heart disease, stroke, arthritis, and some cancers. If you are obese, losing even 5 to 10 percent of your weight can delay or prevent some of these diseases. For example, that means losing 10 to 20 pounds if you weigh 200 pounds.
NIH: National Institute of Diabetes and Digestive and Kidney Diseases The Weight of the Nation: Part 1, 2, & 3

9/19/13 Research suggests obese people often receive inadequate doses of chemotherapy, which can affect their chances of surviving cancer. Obese people are less likely to survive cancer, and one reason may be a surprising inequality: The overweight are under-treated. Doctors often short them on chemotherapy by not basing the dose on size, as they should. They use ideal weight or cap the dose out of fear about how much treatment an obese patient can bear. Yet research shows that bigger people handle chemo better than smaller people do. Even a little less chemo can mean worse odds of survival, and studies suggest that as many as 40 percent of obese cancer patients have been getting less than 85 percent of the right dose for their size. Now, the largest organization of doctors who treat cancer, the American Society of Clinical Oncology, aims to change that. The group has adopted guidelines urging full, weight-based doses for the obese. Don't call it supersizing; it's right-sizing cancer care, said Dr. Gary Lyman, a Duke University oncologist who led the panel that wrote the advice.
See More.... 
June 26, 2013 Obesity is now classified as a disease. This was the final decision at the annual meeting of the American Medical Association (AMA), the organization that represents doctors nationwide. Despite their own Council on Science and Public Health releasing a report earlier in the meeting which indicated that obesity was not a disease process, the AMA House of Delegates took the bold step to vote in opposition to this report.
Taking away the blame For persons who struggle with their weight and the physicians that care for them, this designation of obesity as a disease is seen as a victory. Currently, there are very few resources available to those with obesity as this entity has been viewed as self-induced. The current dogma suggests that obesity can be cured with proper diet and nutrition. Many persons believe that if you are eating the right foods in the proper portion sizes and following a dedicated exercise regimen, you will never become obese. However, science has taught us that while this may be the case for some persons, there is not a “one size fits all” approach to obesity. Studies have shown that hormones in the body such as leptin and ghrelin play a role in the weight status of an individual. These hormones are just a few of the hormones that regulate energy balance in the human body. Leptin, a hormone that is primarily produced by fat, circulates in the bloodstream and communicates with the brain whether or not the body has had enough to eat. For persons that have a higher leptin level, they will tend to eat more as their body does not sense that there is enough food or energy on board. The leptin level varies from person to person. Some studies suggest that blacks are more likely to have a higher leptin level than whites. One such Study indicated that leptin levels were much higher in black women, even after controlling for factors such as weight. The authors suggested that further research into leptin is needed to investigate racial differences in obesity-related diseases. |
